
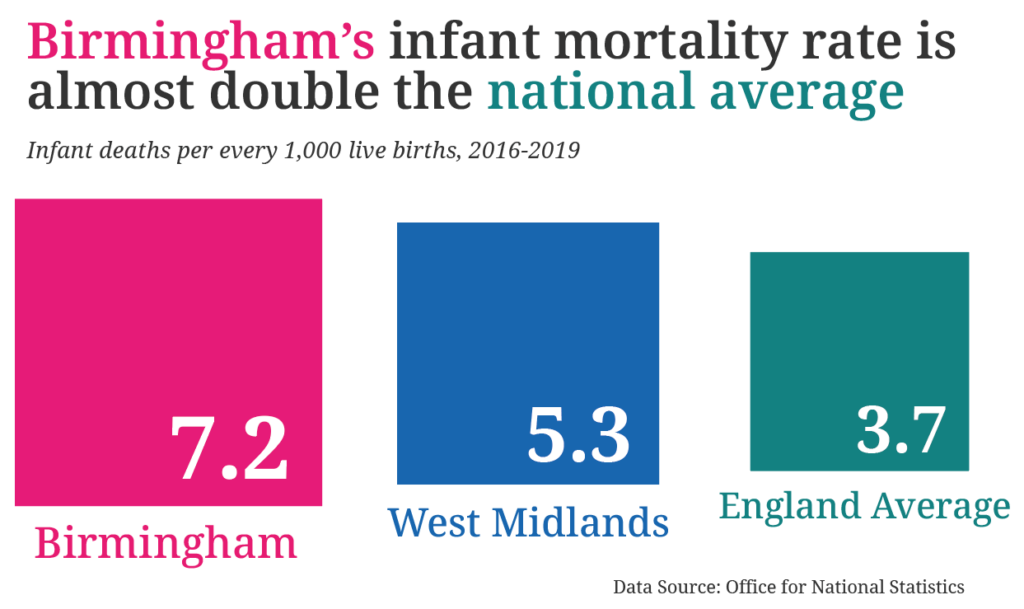
Birmingham City Council has launched a taskforce aimed at reducing the city’s infant mortality rate, which is the highest in England and nearly twice the national average.
Between 2016 and 2019, 472 babies died in Birmingham before their first birthday, according to data from the Office for National Statistics. In comparison, in Merseyside, which has a similar number of annual births, there were only 282 infant deaths.
During a city council meeting, Councillor Paulette Hamilton said the figures were “shocking”.
“We need to do more to prevent the loss of life. The loss of a baby is the most devastating consequence a family could ever face. The fact that in Birmingham our rates are so high is distressing.”
The taskforce follows an inquiry into the city’s high number of baby deaths by the Health and Social Care Scrutiny Committee.
Speaking at the inquiry, Dr Joanna Garstang, Birmingham’s designated doctor for child death, said the city’s high infant mortality rate was not due to failures in maternal care.
Instead, the committee heard that contributing factors included Birmingham’s high level of poverty and above-average obesity rate, and the fact that the city identifies only 30% of growth-restricted babies during pregnancy.

Pakistani babies overrepresented in infant deaths due to genetic conditions
The inquiry also highlighted the city’s high number of infant deaths due to genetic anomalies linked to consanguineous marriage (marriages between first and second cousins), which is a more common practice in the Pakistani community than in the UK’s overall population.
Dr Garstang said that between April 2018 and March 2020, 45% of babies who died in Birmingham due to chromosomal and genetic conditions were from Pakistani families. In comparison only 14% of Birmingham’s population were of Pakistani ethnicity when it was last recorded during the 2011 census.
Speaking to the Birmingham Mail, former regional chief crown prosecutor Nazir Afzal said there was a “strong argument” for outlawing first-cousin marriages to prevent premature deaths and disabilities.
“If there is a direct link between premature death, disability and first cousin marriages [the government] must act on that. It has a duty to protect people’s health.
“The people impacted are the children, and their parents – they are the victims of these choices. It should not be seen as an attack on the community or the family to raise this – it is about protecting vulnerable people and ultimately reducing harm.”

Dr Julie Vogt, a consultant clinical geneticist at the West Midlands Regional Clinical Genetics Service, told the committee that congenital abnormalities occur in 2-3% of pregnancies but that the risk doubles to around 6% for consanguineous couples.
Geneticists can evaluate the case-by-case risk of autosomal recessive diseases, which can occur when both parents carry a recessive gene, and Vogt said more could be done to identify and refer parents who would benefit from genomic diagnostic services.
“It would be important for our service to be accessible,” Vogt said. “In the past a lot of work was done in the community and I think that needs to be rediscovered and re-implemented. [We need] to have hubs in the community of health workers that are particularly interested and motivated to help deliver the service to the local population and particularly the Pakistani community.”
Other contributors to the inquiry agreed that improved genetic literacy and access to genetic services would be beneficial, but emphasised that consanguineous marriages were only one part of Birmingham’s infant mortality problem.
Dr Qulsom Fazil, a lecturer in disability studies and behavioural science at the University of Birmingham, said that in the past, consanguinity had been “a slight scapegoat” and there had been “too much focus on that and not enough focus on other outcomes.”
Chromosomal and genetic conditions were linked to only one in five infant deaths in Birmingham between April 2018 and March 2020 (directly comparable data for England overall is not available).
The committee’s recommendations for reducing non-chromosomal-related infant deaths include improving early detection of poor fetal growth, better support for struggling families, and engaging community groups and faith leaders in a campaign to promote healthy life choices.
‘Ambitious’ target to hit England average by 2025
Councillor Rob Pocock, chair of the Health and Social Care Scrutiny Committee, said that Birmingham’s infant mortality rates had been “stubbornly static” in recent years.
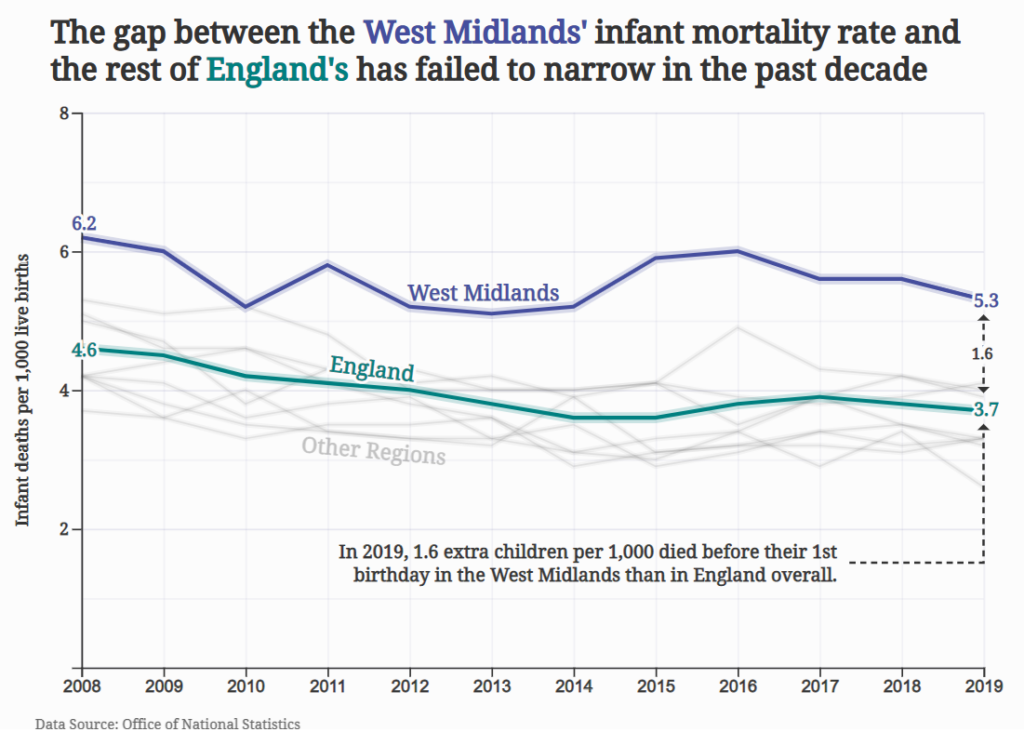
Pocock described the committee’s recommendation of a goal to reduce the city’s rate to the England average by 2025 as “ambitious” but said that something had to be done.
“This is a tragedy that can and must be reduced,” Pocock said. “Something is going wrong. We need to act to put it right.”
Want to learn more:
Read the Health and Social Care Scrutiny Committee’s report here and watch the inquiry sessions here and here.
Watch this BBC Newsnight video on the West Midlands’ high infant mortality rate and autosomal recessive diseases due to consanguineous marriages.
Read this recent report from MBRRACE-UK into perinatal deaths across the UK.
